The Complete Guide to Spine Health: Causes, Symptoms, and Physiotherapy Treatment
You wake up, swing your legs off the bed, and feel it immediately: that dull ache in your lower back, or the stiffness that creeps into your neck before your morning coffee. For many people in Singapore, this is not an occasional inconvenience. It is already becoming a norm. Spine health sits quietly at the core of nearly everything the body does, and when it fails, everything else suffers.
This guide covers the anatomy behind spine problems, the common back pain causes that most patients overlook, the symptoms that signal something needs attention, and how spine physiotherapy addresses the root cause rather than masking discomfort. Whether you are managing a recent flare-up or trying to understand a condition you have lived with for years, the information here is designed to be practical and clear.
What Is Spine Health?
Spine health refers to the proper structure, alignment, and function of the vertebral column and all the tissues surrounding it: the intervertebral discs, spinal nerves, supporting muscles, and ligaments. A healthy spine allows the body to stand upright, move freely in multiple directions, absorb physical load, and protect the spinal cord from injury.
The spine is divided into three regions:
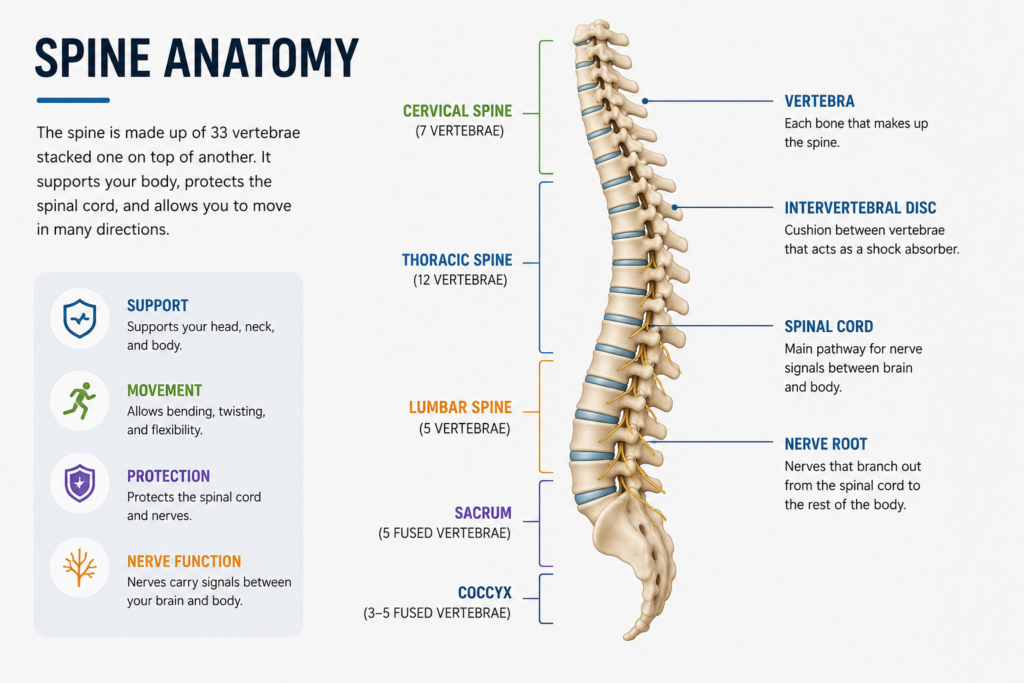
- Cervical spine (neck): seven vertebrae that support the head and allow rotation and side-bending.
- Thoracic spine (mid-back): twelve vertebrae connected to the rib cage, providing stability to the trunk.
- Lumbar spine (lower back): five larger vertebrae that carry the bulk of the body’s weight and enable forward bending and lifting.
Between each vertebra sits an intervertebral disc: a cushion of fibrocartilage that absorbs shock and allows movement. Spinal nerves branch out from the spinal cord at each level, supplying sensation and motor control to the arms, torso, and legs. When any of these structures is compressed, inflamed, or misaligned, the effect travels far beyond the spine itself.
What Are the Most Common Spine Problems?
Spinal conditions vary widely in origin and severity. These are the presentations most frequently seen in clinical practice:
Neck Pain and Cervical Strain
Prolonged phone use and desk work have made cervical strain increasingly prevalent, particularly among younger adults. Sometimes referred to as ‘tech neck’, this pattern involves sustained forward head posture that places excessive load on the cervical vertebrae and surrounding muscles. Pain is typically felt at the base of the skull, across the shoulders, and into the upper back.
Lower Back Pain
Mechanical lower back pain is the most common musculoskeletal complaint globally. Lower back pain causes include muscle strain from improper lifting, disc stress from prolonged sitting, and joint irritation from repetitive movement. Most episodes are not structural in origin, which is precisely why targeted spinal treatment that addresses movement patterns and muscle function is so effective.
Herniated Disc (Slipped Disc)
A herniated disc occurs when the inner gel-like nucleus of an intervertebral disc pushes through a tear in its outer ring. This is commonly called a slipped disc, though the disc does not literally slip out of place. The displaced tissue can press on adjacent nerves, producing sharp, radiating pain, tingling, or weakness.
Sciatica
Sciatica describes pain that travels along the path of the sciatic nerve: from the lower back, through the buttock, and down one leg. It is not a diagnosis in itself but a symptom of nerve compression, most often caused by a herniated lumbar disc or narrowing of the spinal canal (spinal stenosis). The burning or electric quality of sciatic pain is one of the most recognisable presentations in spine care.
Postural Dysfunction
Postural dysfunction develops gradually, over months or years of habitual positioning. Rounded shoulders, a flattened lumbar curve, or a jutting chin are not just aesthetic concerns. Each deviation shifts the load distribution across the spine and creates chronic muscle overactivity in some areas and weaknesses in others. Posture and spine health are inseparable: one directly shapes the other.
Degenerative Spinal Conditions
Age-related changes to the spine, including osteoarthritis of the facet joints and disc degeneration, are part of normal ageing. They do not always cause pain. When they do, physiotherapy focuses on managing load, maintaining mobility, and preventing muscular deconditioning that tends to amplify pain over time.
What Causes Spine Pain and Dysfunction?
Causes of pack pain rarely trace back to a single incident. In most cases, a combination of postural habits, lifestyle factors, and physical conditioning creates a mechanical imbalance that accumulates until the body signals a problem.
- Poor posture and prolonged sitting: Seated posture compresses the lumbar discs and shortens the hip flexors, placing the lower back in a mechanically disadvantaged position for hours at a time.
- Weak core and spinal muscles: The deep stabilising muscles of the trunk (particularly the transverse abdominis and multifidus) are designed to protect the spine during movement. When they are underdeveloped, superficial muscles compensate and fatigue faster.
- Repetitive strain and improper lifting: Bending from the waist rather than the hips, or twisting under load, applies asymmetrical forces to the discs and joints.
- Sedentary lifestyle: Reduced movement decreases circulation to spinal structures, limits the natural fluid exchange that keeps discs healthy, and allows postural muscles to weaken.
- Age-related degeneration: Discs lose water content over time, reducing their capacity to absorb load. Joint cartilage thins. These changes are gradual and manageable with the right approach.
- Stress-related muscle tension: Chronic psychological stress causes sustained muscle guarding, particularly in the neck and upper trapezius. Many patients first notice neck and back pain during periods of high workload or personal pressure.
Taken together, these factors create a mechanical imbalance: the spine is asked to function under a load that cannot be properly distributed, leading to tissue irritation, nerve sensitisation, and eventually pain.
Common Symptoms of Spine Problems
Symptoms vary depending on which spinal region is affected and whether nerve structures are involved. Recognising the pattern helps determine the appropriate path of care:
- Local pain: Aching or sharp pain centered on the neck, mid-back, or lower back, often worsening with sustained postures or specific movements.
- Stiffness and reduced mobility: Difficulty rotating the neck fully, bending forward comfortably, or rising from a seated position without discomfort.
- Radiating pain: Pain that travels from the spine into the arms (from the cervical region) or legs (from the lumbar region), indicating possible nerve involvement.
- Tingling or numbness: Pins-and-needles sensations in the hands, fingers, feet, or toes; a sign of nerve compression or irritation.
- Muscle weakness: Difficulty gripping objects, holding the arm overhead, or controlling leg movement, particularly on one side.
- Postural changes: A visible lean to one side, forward head carriage, or loss of the normal inward curve in the lower back.
Not every symptom is cause for alarm. But symptoms that persist beyond two weeks, or that include tingling, numbness, or weakness, warrant professional assessment rather than continued self-management.
How Do Spine Problems Affect Daily Life?
Singapore’s working culture places considerable physical demand on the spine, often in ways that are not immediately obvious. Office workers sit through long commutes on the MRT and then remain seated for most of the working day. Those in service, construction, and healthcare roles perform repetitive movements or sustained postures across long shifts. Both patterns carry significant spinal load.
The functional impact of spine problems is wide-reaching:
- Difficulty sitting, standing, or walking for extended periods, limiting work capacity and social participation.
- Disrupted sleep from pain that worsens when lying down or prevents comfortable positioning.
- Reduced ability to perform household tasks, exercise, or care for family members.
- Heightened reliance on pain-relief tablets, which manage discomfort but do not address its source.
- Gradual withdrawal from physical activity, which accelerates deconditioning and makes recovery slower.
The longer spinal conditions are left unmanaged, the more entrenched these patterns become. Early intervention shortens the recovery timeline and prevents a short-term problem from becoming a long-term one.
How Does Physiotherapy Treat Spine Conditions?
Spine physiotherapy does not treat pain in isolation. It identifies the mechanical and neuromuscular causes behind a patient’s symptoms and applies specific interventions to correct them. The goal of spinal treatment is to restore function and prevent recurrence, not simply reduce immediate discomfort.
Key treatment methods used in physiotherapy for spine pain include:
Manual Therapy
Manual therapy involves hands-on techniques applied to joints, muscles, and soft tissues. Joint mobilisation restores the range of motion to stiff spinal segments. Soft tissue work reduces muscle guarding and improves local circulation. These techniques are calibrated to the patient’s presentation and are not uniformly forceful; many are gentle and precisely targeted.
Myofascial Release
Myofascial release is a manual technique that applies sustained, gentle pressure to the fascia (the connective tissue that surrounds muscles and organs). When fascia becomes restricted through sustained postures, injury, or inflammation, it can limit movement and contribute to widespread pain patterns. Releasing these restrictions improves tissue mobility and reduces referred discomfort. Patients often describe the sensation as deep pressure that eases progressively, not sharp pain.
Electrotherapy
Electrotherapy uses electrical currents to reduce pain and support tissue healing. TENS (transcutaneous electrical nerve stimulation) modulates pain signals by stimulating nerve pathways. Ultrasound therapy applies sound waves to deeper tissue to reduce inflammation and promote repair. These modalities are used as part of a broader treatment plan, not as standalone interventions.
Movement Correction
Many spinal problems originate in how a person sits, lifts, walks, or performs repeated tasks at work. Movement correction involves analysing these patterns and retraining the body to move with better spinal alignment. This may include gait retraining, seated posture correction, or coaching on specific work tasks. The detail matters: a one-centimeter change in how someone positions their screen can alter the load on their cervical spine across an eight-hour day.
Strengthening Programmes
Progressive strengthening of the core and spinal muscles is one of the most evidence-supported approaches to long-term spine health. Physiotherapy treatment begins with activation of the deep stabilisers and progressively loading the spine in controlled, functional movement patterns. The programme is adapted as the patient’s capacity improves.
Book a consultation at Rapid Physiocare to receive a personalised spinal assessment and treatment plan from our experienced physiotherapists.
What Exercises Can Improve Spine Health?
Exercise is one of the most effective long-term strategies for managing and preventing spine problems. But the type of exercise matters as much as the effort is applied. Random gym sessions or generic ‘back stretches’ found online are not substitutes for a guided programme that accounts for your specific spinal condition, current fitness level, and movement deficits.
Core Strengthening Exercises
Effective core work for spinal rehabilitation targets the deep stabilising muscles first. Exercises such as dead bug variations, bird-dog, and transverse abdominis activation are prescribed before more demanding loaded movements. The reasoning: a spine that cannot be stabilised under light load should not be placed under a heavy one.
Mobility Exercises
Mobility exercises restore movement to stiff spinal segments and surrounding joints. Cat-cow mobilisation, thoracic rotation, and hip flexor lengthening are common starting points. The goal is not extreme flexibility; it is the recovery of the functional range of motion that allows daily tasks to be performed without compensation.
Postural Correction Drills
Postural correction drills retrain the neuromuscular habits that maintain spinal alignment. These are not passive stretches. They are active exercises that teach the body to hold the spine in a more neutral position during sitting, standing, and walking. Chin tucks, scapular retraction exercises, and wall angel drills are frequently prescribed for patients with forward head posture and rounded shoulders.
Stretching Tight Muscles
Muscle tightness in the hip flexors, hamstrings, and thoracic extensors contributes significantly to lower back pain. Targeted stretching addresses these restrictions, but only when applied in the correct sequence for the patient’s condition. Stretching an acutely inflamed muscle, for instance, can worsen rather than relieve pain.
How to Maintain Good Spine Health Daily?
Maintaining spine health between clinic sessions and after discharge depends on consistent daily habits. The following practices are straightforward to implement and clinically meaningful when applied regularly:
Ergonomic Workstation Setup
Set your monitor at eye level. Position the keyboard so your elbows rest at approximately 90°. Use a chair that supports the natural inward curve of the lumbar spine.
Feet should be flat on the ground or on a footrest. Avoid resting the wrist on a hard surface while typing, as this creates upstream tension through the forearm, shoulder, and neck.
Regular Movement Breaks
The spine is not designed for sustained static loading. Standing, walking briefly, or performing simple spinal movements every 45 to 60 minutes reduces disc pressure, improves circulation, and prevents the muscle fatigue that accumulates in fixed postures. A short walk to the pantry counts. Consistency matters more than duration.
Proper Lifting Technique
When lifting from the floor, hinge at the hips and bend the knees rather than rounding the lower back. Keep the load close to the body. Avoid twisting at the waist while holding weight. These mechanics apply to grocery bags as much as they do to heavy boxes at work.
Sleeping Posture
Side sleeping with a pillow between the knees maintains pelvic alignment and reduces rotational stress on the lumbar spine. Back sleeping with a pillow under the knees achieves a similar effect. Sleeping on the stomach is generally discouraged for patients with neck or lower back conditions, as it places the cervical spine in sustained rotation.
Physical Activity
Sustained aerobic activity, whether swimming, cycling, walking, or low-impact group exercise, supports spinal health by maintaining cardiovascular fitness, managing weight, and preserving disc hydration through movement. Patients recovering from spinal conditions should discuss activity selection with their physiotherapist before resuming intense exercise.
Speak with a Rapid Physiocare physiotherapist to develop a personalised spine health maintenance plan suited to your work and lifestyle.
Can Spine Problems Be Prevented?
Yes, in many cases. Prevention does not mean eliminating all spinal stress; that is neither possible nor desirable. The spine is built to move and bear load. Prevention means ensuring it has the muscular support, range of motion, and movement habits to handle daily demands without progressive tissue breakdown.
Physiotherapy for the spine is not solely a reactive intervention. Many patients benefit from periodic reviews to identify early postural or movement changes before they become symptomatic. Catching a developing muscle imbalance or reduced spinal mobility at three months is considerably easier to address than the same imbalance at three years.
Early correction also changes the long-term trajectory. A patient who addresses neck and back pain at the first recurrence is less likely to develop a chronic pain pattern than one who waits until the condition significantly limits daily function. The window for straightforward intervention is wider early on.
When Should You See a Physiotherapist?
Seek a professional assessment if you experience any of the following:
- Pain that has persisted for more than one to two weeks without improvement.
- Pain that radiates from the spine into the arm or leg.
- Tingling, numbness, or weakness in the arms, hands, legs, or feet.
- Episodes of spine pain that recur every few weeks or months.
- Difficulty performing routine tasks such as dressing, sitting through meals, or sleeping through the night.
- Pain that is worsening rather than settling with rest.
These are not red flags that signal something catastrophic. They are clinical indicators that the body has exceeded its capacity to self-correct and that structured physiotherapy for spine pain is likely to produce a faster, more complete recovery than continued rest.
Take the First Step Towards Better Spine Health
Spine problems rarely resolve on their own when the underlying causes remain unchanged. The posture, the movement habits, the muscle imbalances: these persist until something directly addresses them. That is what spine physiotherapy is designed to do.
At Rapid Physiocare, our physiotherapists assess the full picture: not just where the pain is, but why it is there. With six clinics across Singapore and 45 years of combined clinical experience, the team brings specific expertise in spinal conditions, postural assessment, and rehabilitation. Every treatment plan is built around your condition, your goals, and your daily life.
Spinal treatment works best when it begins early. Do not wait for a manageable problem to become a chronic one.
Book a consultation at Rapid Physiocare today. Walk in with pain. Walk out with a plan.
Frequently Asked Questions.
What are the most common causes of spine pain?
Poor posture, prolonged sitting, weak core muscles, repetitive strain, improper lifting, and age-related disc degeneration are the leading causes of spine pain.
How do I know if my back pain is serious?
Seek assessment if pain persists beyond two weeks, radiates into the leg or arm, or is accompanied by numbness, tingling, or muscle weakness.
Can physiotherapy help treat spine problems?
Yes. Physiotherapy treats the root cause through manual therapy, targeted exercises, movement correction, and electrotherapy to restore function and reduce pain.
What exercises are best for improving spine health?
Core stabilisation exercises, mobility drills, postural correction work, and targeted muscle stretching form the foundation of a guided spine rehabilitation programme.
How can I improve my posture to reduce spine pain?
Set your monitor at eye level, support your lumbar curve when seated, take movement breaks every 45 to 60 minutes, and strengthen your deep spinal stabilisers.
Is it safe to exercise with back or spine pain?
In most cases, yes, with guidance. A physiotherapist will identify which movements are safe and prescribe exercises that support recovery without aggravating the injury.
Can spine problems go away on their own?
Minor muscle strain often resolves within two weeks. Structural issues such as disc herniation or nerve compression require professional assessment and targeted treatment.
How can I prevent spine-related problems in daily life?
Maintain an ergonomic workstation, lift correctly by hinging at the hips, move regularly, sleep with spinal alignment supported, and strengthen your core consistently.
When should I see a physiotherapist for spine pain?
See a physiotherapist if pain persists beyond two weeks, recurs frequently, limits daily tasks, or involves radiating pain, tingling, or weakness in the limbs.
Tags : spine care Singapore


