The Complete Guide to Osteoarthritis: Causes, Symptoms, and Physiotherapy Treatment
That stiffness in your knee when you get up from your desk after a long meeting. The subtle grinding you feel climbing the stairs. The hip that aches after a two-hour flight. Most people chalk these up to getting older, push through them, and carry on.
But these are not signs to ignore. They are the early signals of cartilage degeneration: a process that, once underway, does not reverse on its own. The good news is that physiotherapy for osteoarthritis, when started early, gives your joints the best chance at lasting function. This guide covers what you need to understand about osteoarthritis treatment, from causes to symptoms to a phased recovery plan.
What Is Osteoarthritis?
Osteoarthritis is a degenerative joint disease. Osteoarthritis is a degenerative joint condition affecting millions worldwide. According to the WHO, osteoarthritis is one of the most common joint disorders worldwide. It occurs when the cartilage protecting the ends of your bones gradually wears down, reducing the cushioning between joint surfaces. As cartilage breaks down, bones begin to bear more of the mechanical load. Over time, this leads to bone friction in joints, inflammation, and structural changes to the joint itself.
It is the most common form of arthritis and affects multiple joints across the body: knees, hips, shoulders, spine, hands, and fingers. It is progressive, meaning the joint does not recover spontaneously. But progression is not inevitable. The rate at which osteoarthritis advances depends heavily on how early it is identified and how consistently it is managed.
Why Does Osteoarthritis Develop?
Osteoarthritis does not have a single cause. It develops from a combination of biological and mechanical factors that accumulate over the years.
Age-related joint changes are the most common contributing factor. As the body ages, the capacity to regenerate cartilage tissue slows. But age alone does not cause osteoarthritis. Many of the patients seen at Rapid Physiocare’s six clinic locations develop symptoms earlier than expected, largely due to lifestyle factors.
The key osteoarthritis causes include:
- Previous joint injuries that altered loading patterns.
- Repetitive joint stress from occupational or recreational activities.
- Increased body weight, which raises compressive load on the knees and hips.
- Genetics and family history of degenerative joint disease.
- Poor posture and joint alignment that distribute force unevenly across cartilage.
- Muscle weakness around joints, which transfers excess load to joint structures.
Singapore’s work culture plays a direct role here. Hours of sustained sitting in a fixed lumbar position, combined with minimal load-bearing physical activity, weaken the muscles that stabilise major joints. When those muscles cannot absorb force effectively, the cartilage takes it instead.
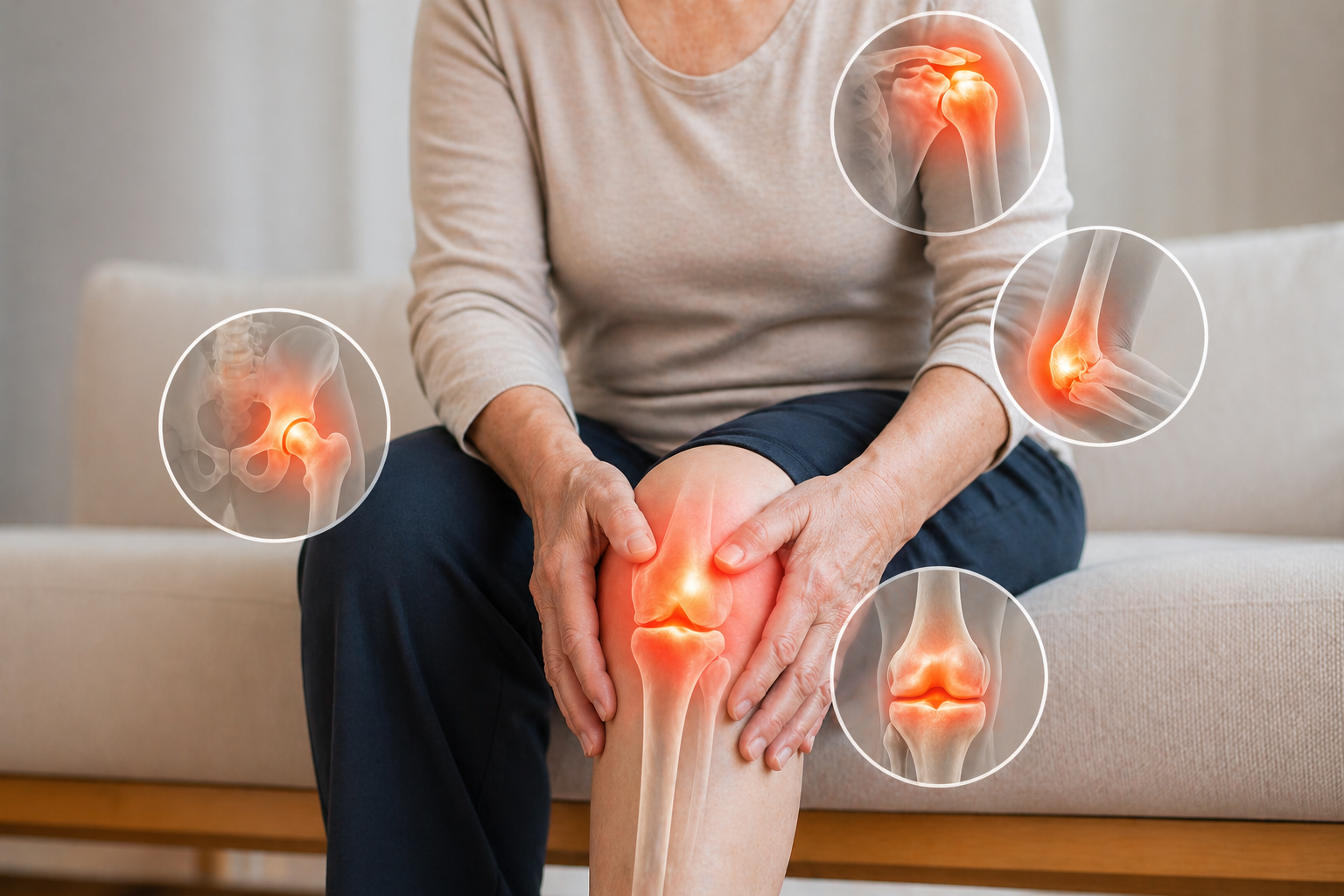
Which Joints Are Commonly Affected?
Osteoarthritis can develop in almost any joint, but certain joints bear greater mechanical demand and are therefore more vulnerable.
Knee Osteoarthritis
Knee osteoarthritis is the most common presentation. Patients typically report pain during walking, difficulty climbing stairs, and joint stiffness that worsens after rest. The medial compartment of the knee (the inner side) is usually affected first, producing a characteristic inward bow in advanced cases. Knee joint pain physiotherapy targets the quadriceps and hamstrings to reduce compressive load and restore tracking of the patella.
Hip Osteoarthritis
Hip osteoarthritis symptoms present as deep, aching pain in the groin or outer hip, often mistaken for a muscular strain. Patients notice difficulty walking long distances, reduced stride length, and stiffness after sitting for extended periods. What is often missed clinically: hip pain. Osteoarthritis frequently causes referred pain into the knee, leading to delayed diagnosis.
Shoulder Osteoarthritis
Less common but functionally limiting. Physiotherapy addresses the loss of range in overhead and rotational movements. Pain is typically dull at rest and sharp during reaching or lifting.
Cervical and Lumbar Spine Osteoarthritis
The facet joints and intervertebral discs of the spine are vulnerable to degenerative change. Cervical osteoarthritis produces neck stiffness, headaches, and occasionally arm pain if nerve roots are involved. Lumbar osteoarthritis creates lower back stiffness, particularly in the morning, and may radiate into the buttocks or thighs. Prolonged desk work may accelerate this.
Hand and Finger Osteoarthritis
Joint swelling, tenderness at the base of the thumb, and grip weakness are the most common complaints. Fine motor tasks, such as opening jars or typing for long periods, become progressively harder.
What Are the Early Symptoms of Osteoarthritis?
Early-stage osteoarthritis is frequently dismissed because the symptoms are intermittent. They appear after activity and resolve with rest, which gives the impression that nothing serious is happening. But this is precisely when intervention matters most.
Watch for these osteoarthritis symptoms:
- Stiff joints in the morning that ease within 30 minutes of movement.
- Joint stiffness after rest, such as after sitting through a long meeting or a car commute.
- Pain during movement, particularly at the end range of a joint’s motion.
- Clicking or grinding sensations (crepitus) in the knee or shoulder during movement.
- Joint swelling and stiffness that appear after sustained activity.
- Reduced range of motion that limits everyday tasks like bending, squatting, or reaching.
The 30-minute rule is clinically significant: morning stiffness lasting longer than 30 minutes suggests inflammatory arthritis rather than osteoarthritis and warrants a different diagnostic approach. With osteoarthritis, stiffness typically resolves quickly once you start moving.
How Does Osteoarthritis Progress Over Time?
Osteoarthritis is staged by symptom severity and functional impact, not by age.
Early stage: Mild discomfort during or after physical activity. Joint space narrowing is minimal. Physiotherapy at this stage produces the most favourable outcomes.
Moderate stage: Persistent joint stiffness, activity limitation, and pain during movement that no longer fully resolves with rest. Muscle weakness around joints becomes more pronounced as patients unconsciously avoid movements that provoke pain, accelerating deconditioning.
Advanced stage: Chronic joint pain treatment becomes the primary goal. Significant loss of joint mobility, difficulty with weight-bearing activities, and disrupted sleep. At this stage, physiotherapy focuses on maintaining function and slowing further degeneration.
Rest alone does not resolve the underlying cause at any stage.
How Is Osteoarthritis Diagnosed?
Physiotherapists at Rapid Physiocare use a structured clinical assessment to confirm osteoarthritis and understand how it is affecting your specific joint mechanics.
This includes:
- A detailed movement analysis to identify compensatory loading patterns.
- Physical assessment of joint range, strength, and stability.
- A thorough medical and activity history.
- Referral for imaging (X-ray or MRI) when clinical findings indicate joint space narrowing or structural change.
The clinical assessment matters as much as the imaging. An X-ray shows structural change; a physiotherapist identifies how that change is affecting the way you move. Both are necessary to design an effective treatment plan.
How Does Osteoarthritis Affect Daily Life?
The functional impact of osteoarthritis extends well beyond the joint itself.
Patients describe difficulty walking more than one MRT stop, avoiding stairs at Orchard Road because of the pain, or waking at 3 am due to joint discomfort when shifting position. Social withdrawal follows. Recreational activities like morning walks at East Coast Park or weekend cycling get progressively reduced. Over time, reduced physical activity leads to weight gain, which increases joint load further.
Pain in multiple joints compounds this: when the knee is compensated for by shifting weight to the opposite hip, that hip begins to experience abnormal mechanical stress. This cascade of compensatory movement patterns is one of the most important reasons to seek joint pain treatment early.
What Are the Best Physiotherapy Treatments for Osteoarthritis?
Physiotherapy for osteoarthritis focuses on reducing pain, restoring joint function, and preventing further cartilage degeneration. No two presentations are identical; treatment at Rapid Physiocare follows no generic protocols.
The approach is structured across three phases.
Phase 1: Acute Phase (Pain Relief)
The immediate priority is reducing joint inflammation and offloading painful structures. This phase uses:
- Manual therapy and joint mobilisation to restore the basic range of motion and reduce stiffness.
- Myofascial release to address muscle tightness that is compressing the joint.
- Electrotherapy to modulate pain signals and reduce swelling.
- Education on activity modification: which movements to avoid temporarily and which to continue.
Phase 2: Subacute Phase (Restoring Range of Motion)
Once pain is managed, the focus shifts to loss of joint mobility. This phase introduces:
- Progressive range-of-motion exercises specific to the affected joint.
- Posture and joint alignment correction to recalibrate loading patterns.
- Neuromuscular retraining to regain normal movement coordination.
- Functional movement training that mirrors the tasks you need to perform daily.
Phase 3: Recovery Phase (Strength and Prevention)
The final phase builds the muscular support system around the joint to reduce the load cartilage must absorb. This includes:
- Targeted strengthening of muscles that stabilise the affected joint (gluteus medius for hip, quadriceps and VMO for the knee; rotator cuff for the shoulder).
- Exercise for joint health that is load-appropriate and progressed carefully.
- Education on how to prevent osteoarthritis from advancing.
- A long-term home exercise programme.
With 45 years of combined clinical experience across six locations, the team at Rapid Physiocare structures these phases based on your assessment findings, not a standard template.
What Exercises Help Manage Osteoarthritis?
Exercise is one of the most evidence-supported interventions for managing osteoarthritis. The key is selecting the right type, at the right intensity, at the right phase of recovery.
Safe and effective options include:
- Low-impact strengthening exercises: water-based resistance, seated leg press, and wall squats at shallow angles.
- Range-of-motion exercises: gentle joint circles, assisted stretches, supine hip mobility work.
- Functional movement training: step-ups, sit-to-stand progressions, corridor walking drills.
- Stretching routines for the muscles that cross the affected joint improve both mobility and load distribution.
A safety note: exercise for joint pain relief should be guided by a physiotherapist in the early stages. Self-prescribed exercise that uses the wrong load or range can accelerate cartilage wear rather than protect against it.
Can Osteoarthritis Be Managed Without Surgery?
Yes. For most patients, particularly those presenting in the early and moderate stages, osteoarthritis treatment through physiotherapy and lifestyle modification produces meaningful, lasting improvements without surgical intervention.
Surgery (typically joint replacement) is considered when conservative management has been exhausted, and quality of life is severely compromised. Physiotherapy has been shown to delay or, in many cases, eliminate the need for surgery by restoring joint mechanics, reducing pain, and strengthening the supportive musculature.
Lifestyle changes for arthritis that support conservative management include:
- Weight management: Reducing body weight by 5 to 10% measurably decreases compressive load on the knees.
- Activity modification: Replacing high-impact activities with low-impact alternatives that preserve cardiovascular fitness.
- Sleep and recovery: Adequate sleep supports the body’s capacity to manage inflammation.
The window for effective conservative care is wide. But it narrows as the disease progresses.
How to Prevent Osteoarthritis Progression
Osteoarthritis cannot be reversed once cartilage is lost. But its progression can be slowed significantly with consistent intervention.
Joint pain prevention tips that are clinically supported:
- Maintain a healthy body weight to reduce compressive joint load.
- Stay physically active with low-impact exercise for joint health (swimming, cycling, walking).
- Strengthen the muscles surrounding your most-used joints before symptoms develop.
- Correct sitting posture and workstation ergonomics, particularly for those working long hours at a desk.
- Avoid sustained positions that compress a single joint repeatedly (e.g., prolonged kneeling or deep squatting without adequate strength).
The earlier these habits are established, the more cartilage there is to protect.
When Should You See a Physiotherapist?
Do not wait for the pain to become constant before seeking assessment.
Seek physiotherapy for joint pain if you notice:
- Joint stiffness that persists beyond 30 minutes in the morning.
- Pain during movement that limits a specific activity you previously managed without difficulty.
- A change in how you walk, sit, or carry weight, even if subtle.
- Joint swelling that reappears after physical activity.
- Persistent joint pain after sitting for more than 45 minutes.
Early assessment gives the physiotherapist the best opportunity to intervene before compensatory movement patterns become habitual. Habitual compensation is harder to unlearn than the original problem.
Why Choose Physiotherapy for Osteoarthritis?
Physiotherapy is non-invasive, evidence-based, and addresses the root mechanical causes of osteoarthritis rather than masking symptoms.
It reduces dependency on tablets over time and improves function in ways that a pain reliever cannot: by rebuilding the strength, range, and coordination that protect the joint during daily activity. It produces results that are durable, not temporary, because the changes happen at the level of muscle, movement pattern, and joint mechanics.
Rapid Physiocare’s six clinic locations across Singapore provide access to physiotherapists with 45 years of combined clinical experience in managing osteoarthritis at every stage. Each treatment plan is based on your assessment results. No generic protocols. No guesswork.
Take the first step to better joint health.
If morning stiffness, joint pain while walking, or reduced mobility are affecting your daily life, a clinical assessment is the right starting point. The physiotherapists at Rapid Physiocare will assess your joint function, identify the contributing factors, and design a phased treatment plan specific to your presentation.
Book a consultation at Rapid Physiocare today to receive a personalised assessment
Frequently Asked Questions
What is osteoarthritis physiotherapy?
Osteoarthritis physiotherapy uses manual therapy, targeted exercise, and movement retraining to reduce joint pain, restore range of motion, and slow cartilage degeneration without surgery.
What is the main cause of osteoarthritis?
Osteoarthritis is caused by cumulative cartilage wear from aging, joint injuries, excess body weight, poor biomechanics, and muscle weakness that transfers load onto joint surfaces over time.
Can osteoarthritis be reversed?
Cartilage loss cannot be reversed. But physiotherapy and lifestyle changes can significantly slow progression, reduce pain, and restore function, often avoiding the need for joint replacement surgery.
Is physiotherapy effective for osteoarthritis?
Yes. Physiotherapy is one of the most evidence-supported treatments for osteoarthritis. It reduces pain, improves joint mobility, and strengthens supporting muscles to protect remaining cartilage.
Which joints are most affected by osteoarthritis?
The knee is most commonly affected, followed by the hip, spine, shoulder, and hand joints. Desk-related posture and sedentary habits increase risk in the spine, hip, and knee.
How long does osteoarthritis treatment take?
Most patients see meaningful improvement within 6 to 12 weeks of structured physiotherapy. Full recovery timelines depend on the stage of osteoarthritis, joint affected, and the consistency of the exercise program.
Is exercise safe for osteoarthritis?
Yes, when guided by a physiotherapist. Low-impact strengthening and range-of-motion exercises reduce joint load and pain. Unsupervised high-impact exercise at the wrong stage can worsen cartilage damage.
When should I seek treatment for osteoarthritis?
Seek assessment when you notice persistent morning joint stiffness, pain during movement, reduced range of motion, or changes in the way you walk or sit. Earlier assessment produces better outcomes.
Can young people get osteoarthritis?
Yes. While more common with age, osteoarthritis can develop in younger adults following joint injuries, repetitive occupational strain, or with genetic predisposition. Post-traumatic knee osteoarthritis is well-documented in athletes.
Tags : Osteoarthritis